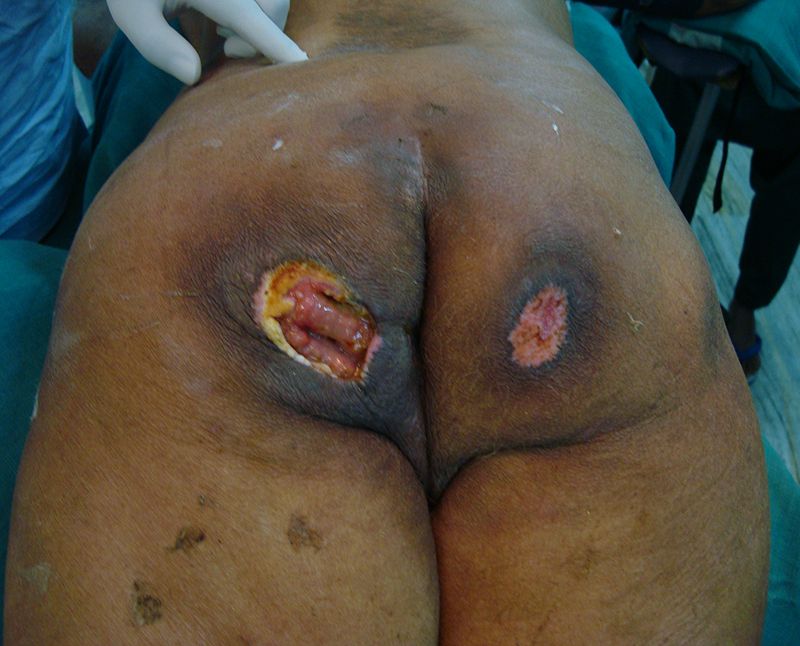
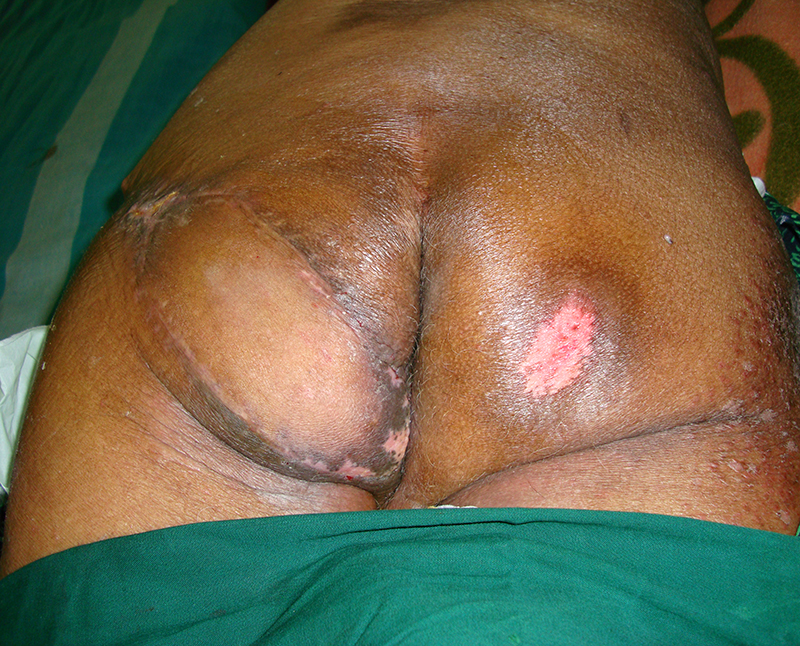
PRESSURE SORE
INTRODUCTION:
Pressure sore, also, known as bed sore or decubitus ulcer is a chronic wound caused by prolonged pressure over skin and other tissues causing tissue ischemia, and preventing lymphatic drainage. It is most commonly seen in lower back and buttocks but can occur on the back of head and heel.
Constant pressure along with friction and moisture can cause pressure ulcers. Bed sores are common in paralyzed persons due to lack of sensation and inability to move by self. Often these persons will be having incontinence of bowel and bladder. Moisture, acidic pH and bacteria in urine and stool increase the chance of development of a bed sore.
‘Prevention is better than cure’ are the golden words in case of pressure sores. While small bedsores any heal by itself, may require surgical interventions.
PROCEDURE
the treatment of pressure sore is usually time consuming and multifactorial.
Pressure sore have been graded to four grades-
- Grade I- skin discoloration with intact skin
- Grade II- some skin loss or damage involving the superficial layers of skin.
- Grade III- necrotic skin patch upto the subcutaneous tissue
- Grade IV- necrosis of skin and underlying structures upto tendon, bone or joint.
NON-SURGICAL MANAGEMENT:
- Identifying risk factors and the patient at risk.
- Positional changes- patients who spend most of their time in bed are advised to change their positions by self or by caregivers every two hours. Wheel chair bound patients are advised to shift their positions every 15min or so.
- Skin Care: daily skin care and assessment of the skin around the areas at risk by educating the care provider
- Diet and lifestyle changes- most patient that develop pressure sores are nutritionally deficient either due to associated co-morbidities or due to higher requirements for tissue healing. Cessation of smoking, good hygiene habits and maintaining activity levels as possible.
- Special mattresses to reduce pressure points.
SURGICAL MANAGEMENT:
It assures increased blood flow to the wound. It, also, removes exudates and thus decreases swelling and infection and wound contracture facilitating wound closure.
- DEBRIDEMENT- The first step in the management of a pressure ulcer includes removal of all dead and devitalized tissue and biofilm. The goal is to create a healthy lining throughout the ulcer cavity. For superficial ulcers, this may be enough, causing the wound to contract and epithelialise, usually as in grade II ulcers
- SOFT TISSUE RECONSTRUCTION- using flaps to provide adequate cushion over pressure point and prevent recurrence. The patient should be adequately nourished and control of other co-morbidities if any. Composite local tissue flaps are most commonly used and the choice of tissue is individualized depending upon the location and depth of ulcer. Flaps are planned so that suture lines are always away from pressure points. Well vsacularised flaps also help in control of infection especially with osteomyelitis.
Ischial Ulcers- first step includes removal of all dead and devitalized tissue and bursa upto the ischial tuberosity including removal of the periosteum, usually done ‘en bloc’. The semitendinous, semimembranous, biceps femoris and gluteus maximus are the most commonly used muscle flaps raised to cover the ischial tuberosity. A posterior thigh skin flap medially or laterally based is raised to cover the muscle and defect. The benefit of the long posterior thigh flap is that it may be raised again in case of recurrence, especially in patients with spinal cord injuries.
Sacral Ulcers- early ulcers may be debrided and split thickness graft applied. Delayed presentations requires rotation flap covers with or without coccygectomy, partial sacrectomy.
Trochanteric Ulcers- early ulcers may be managed with debridement and skin grafting. Deeper ulcers with large areas require flap covers. Bipedicled advancement flap based on fascia lata or the tensor fascia lata, pedicled flaps are commonly used. Anterior based fascio-cutaneous transposition flap wherein the fascia lata is lifted along with the skin and subcutaneous tissue as an anterolateral thigh flap and transposed posteriorly to cover the defect.
Heel pad ulcers- These ulcers are treated with caution and conservatively and treatment approach differs from that of pelvic pressure sores. The major limiting factor is the requirement of offloading of the foot and compromised vascularity to the foot and heel pad per se. Requires offloading of the heel pad.
Negative pressure wound therapy has found merit in treating the heel pad ulcers.
Aggressive management of heel ulcers is limited to a well perfused patient, patient with osteomyelitis and advanced infection which may lead to sepsis or amputation.
RECOVERY:
Recovery takes about 4-6weeks due to chronic nature of the ulcer and poor general nutritional status and associated co-morbidities.
Following flap surgeries for pelvic ulcers, weight bearing on the side of the ulcer is delayed upto 6-8weeks to ensure complete healing especially in case of paraplegics with recurrent ulcers. Early ambulation when possible, without weight bearing on the affected side is the norm.
CASE 1
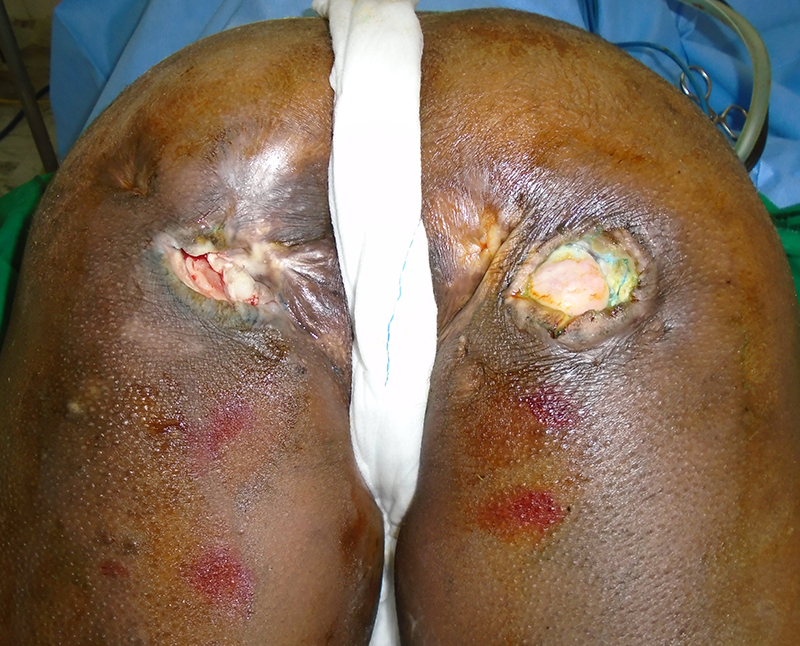
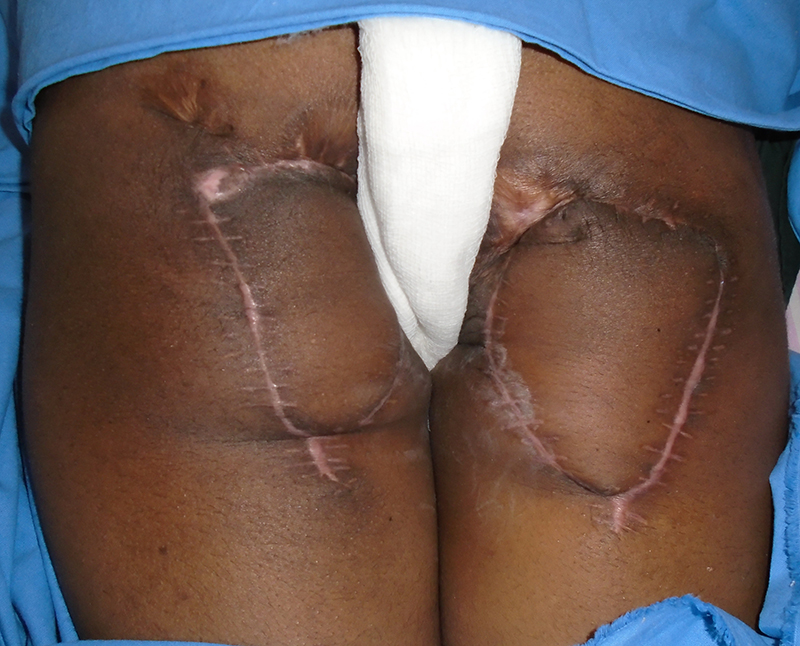
CASE 2